Melatonin Use and Poisoning Reports Surging in Children, Revealing Concerning Problem
Experts believe the cause of the increase in poisoning reports may extend beyond issues of melatonin safety.

Insomnia and melatonin supplementation are not words one would often associate with children.
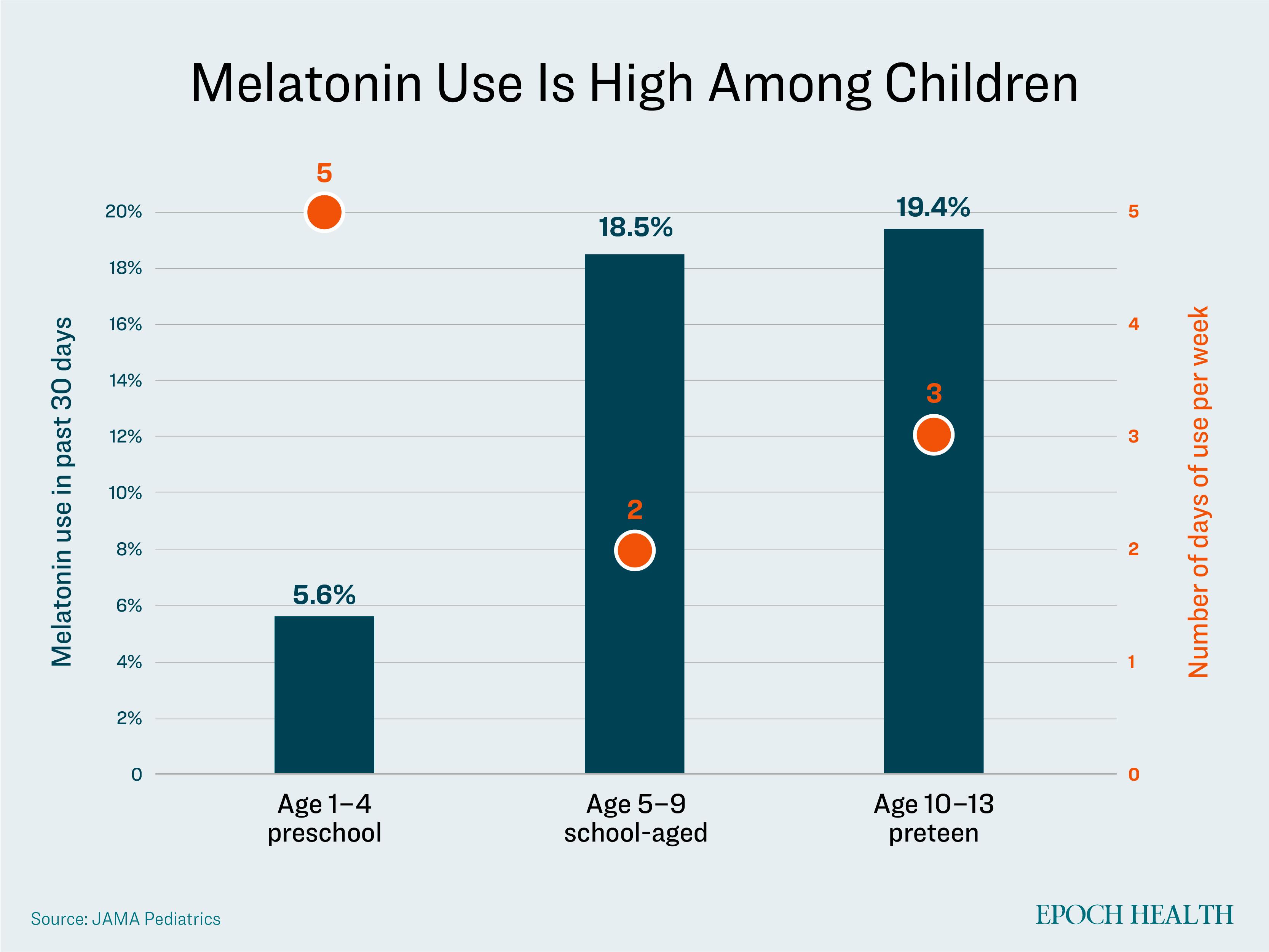
Around one-fifth of American children use melatonin for sleep, with some parents beginning administration to their children at the early age of 1, the authors wrote.
The United States has seen a rapid rise in pediatric melatonin use due to sleep problems. Some clinicians attribute these sleep problems to an increase in mental illness and screen use.
The JAMA Pediatrics study authors compared this finding to their own research results, reporting that the current data indicate a rise in use of about 20 percent. Parents surveyed also reported that their children take the supplement on average two to five days per week, and many take it daily.
Insufficient Sleep Is Common Among Children
“A lot of people think that kids don’t have sleeping problems, and that is absolutely not true,” sleep medicine pediatrician Dr. Gayln Perry, CEO of the Perry Center for Pediatric & Adult Sleep Care, told The Epoch Times.Kids have always had sleeping problems, and these don’t differ much from those of adults.

Just as stress, anxiety, and depression can cause insomnia in adults, the same can occur in children who have different worries from day to day. These may include schoolwork, pressure from peers, and social media interactions.
Many teenagers are also over-committed in their school activities, which impacts their ability to get to bed on time.
Additionally, homeschooling during the pandemic increased children’s screen time. Screens are highly stimulating; their light can suppress and disrupt the sleep cycle.
There is a significant problem with electronics in general, “to the point that some parents really have lost control,” Dr. Perry said. Kids may get up in the middle of the night or early in the morning before school to get on their tablets or phones or to play video games.
Pediatrician Dr. Derek Husmann said he believes screen use is the main problem causing disordered sleeping in children.
A Cheap and Accessible Sleep Aid
Parents and caretakers have, therefore, turned to melatonin.Supplements for children are accessible, unregulated, and can be bought without a prescription. Available in the form of gummies and liquids, they are also appealing to young children.
“The majority of parents that come into my clinic have at least tried melatonin, or the child is already on melatonin—either per recommendation from a general pediatrician or on their own,” Dr. Perry said.
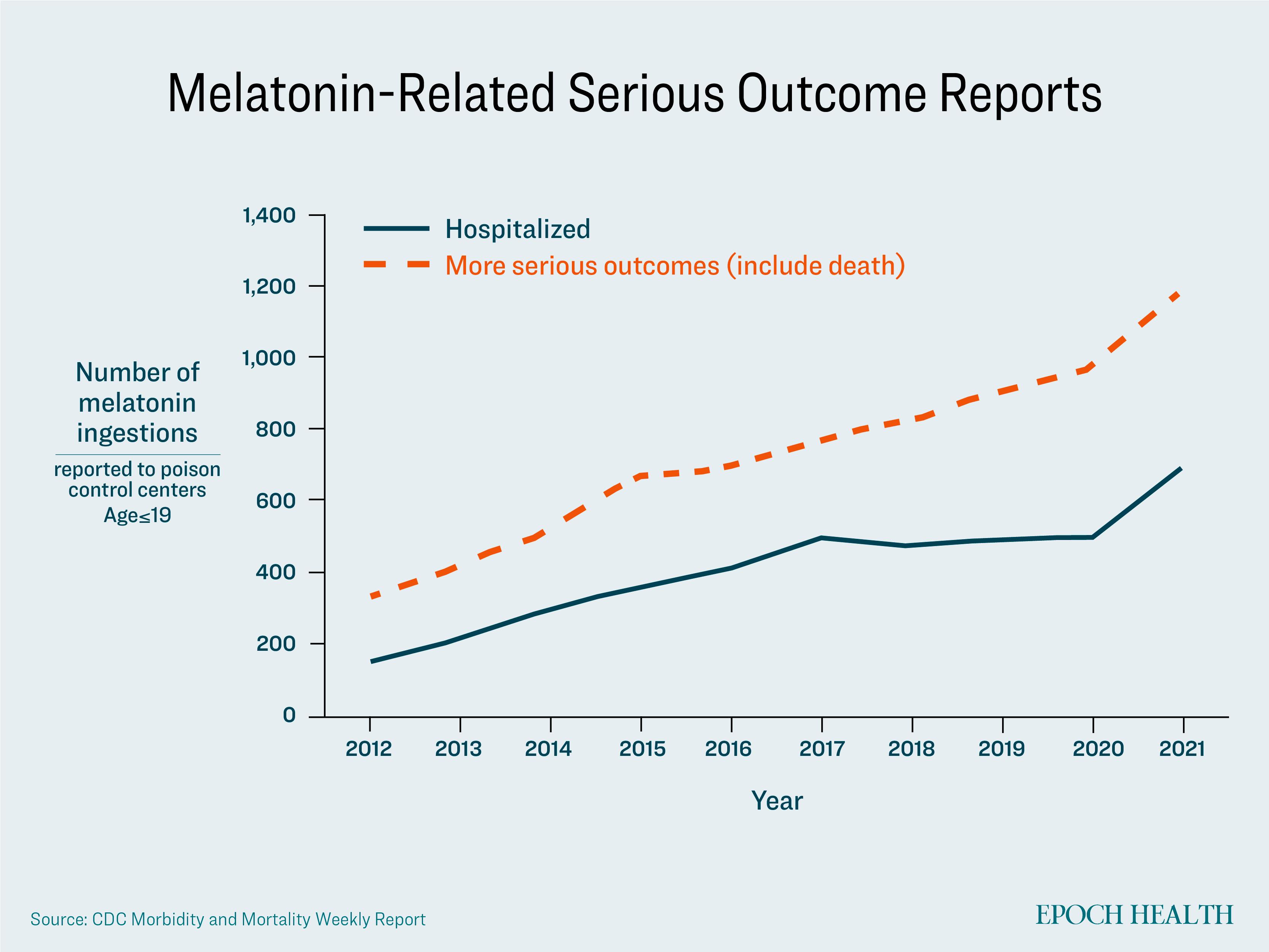
Between 2016 and 2020, sales of melatonin supplements increased by around 150 percent, according to the MMWR.

Melatonin is a natural hormone the body produces to regulate the sleep-wake cycle. Light suppresses, while darkness stimulates the release of melatonin from the pineal gland.
Generally, melatonin supplements are advised to be taken one to two hours before bedtime to mimic the natural cycle.
Melatonin’s effects only last about two hours. “It’s going to facilitate falling asleep quicker, but it’s not going to be around long enough to impact sleep quality,” said Dr. Perry. While parents typically report a short-term benefit when administering melatonin, as time passes, the supplements may not work as well, and the dose may need to be increased.
Dr. Husmann has seen this in his patients.
“It used to bother me a lot when I came across those patients that have been on it for months and months. I asked them to try to wean their kids off ... but there are some cases where they try, and it’s not particularly successful,” he said.
The Dangers
Doctors also generally do not recommend melatonin supplementation for healthy children under age 3 since difficulties falling and staying asleep in these children are almost always behavioral in nature. Yet there have been numerous cases of melatonin use in infants and toddlers.High melatonin levels have also been detected in deceased children.
One case was of a 3-month-old girl routinely given eight to 10 daily doses of 5 milligrams of melatonin supplements as a sleep aid. Such a dosage is well above what’s recommended for a child of any age. The child’s cause of death was inconclusive.
Doctors still do not know why melatonin supplementation may be associated with death, given its assumed high safety profile. It should also be noted that deaths from melatonin supplements make up only a very small percentage of all melatonin poisoning reports.
Dr. Perry said she has never had a patient die from melatonin and expects that since melatonin is an endogenous hormone—meaning it naturally occurs in the body—it should have a wide safety margin.
“I don’t see a lot of downsides other than I wish so many kids didn’t need it in the first place,” Dr. Husmann agreed.
However, Dr. Rishi argued that melatonin is a drug, meaning that it changes a person’s mental or physical state and, therefore, should be treated as such.


Potential Deeper Cause for Concern
Overdosing and consuming contaminated products are established risks of taking store-bought melatonin supplements.Since melatonin is sold as a supplement, it does not have the same regulatory oversight from the U.S. Food and Drug Administration (FDA) as other over-the-counter medications, Dr. Rishi wrote via email. Contamination and variability in dosage are rampant.
Children only require a very low dose of melatonin—around 0.05 to 3 milligrams—but doses from supplements can vary, even among the same batch.
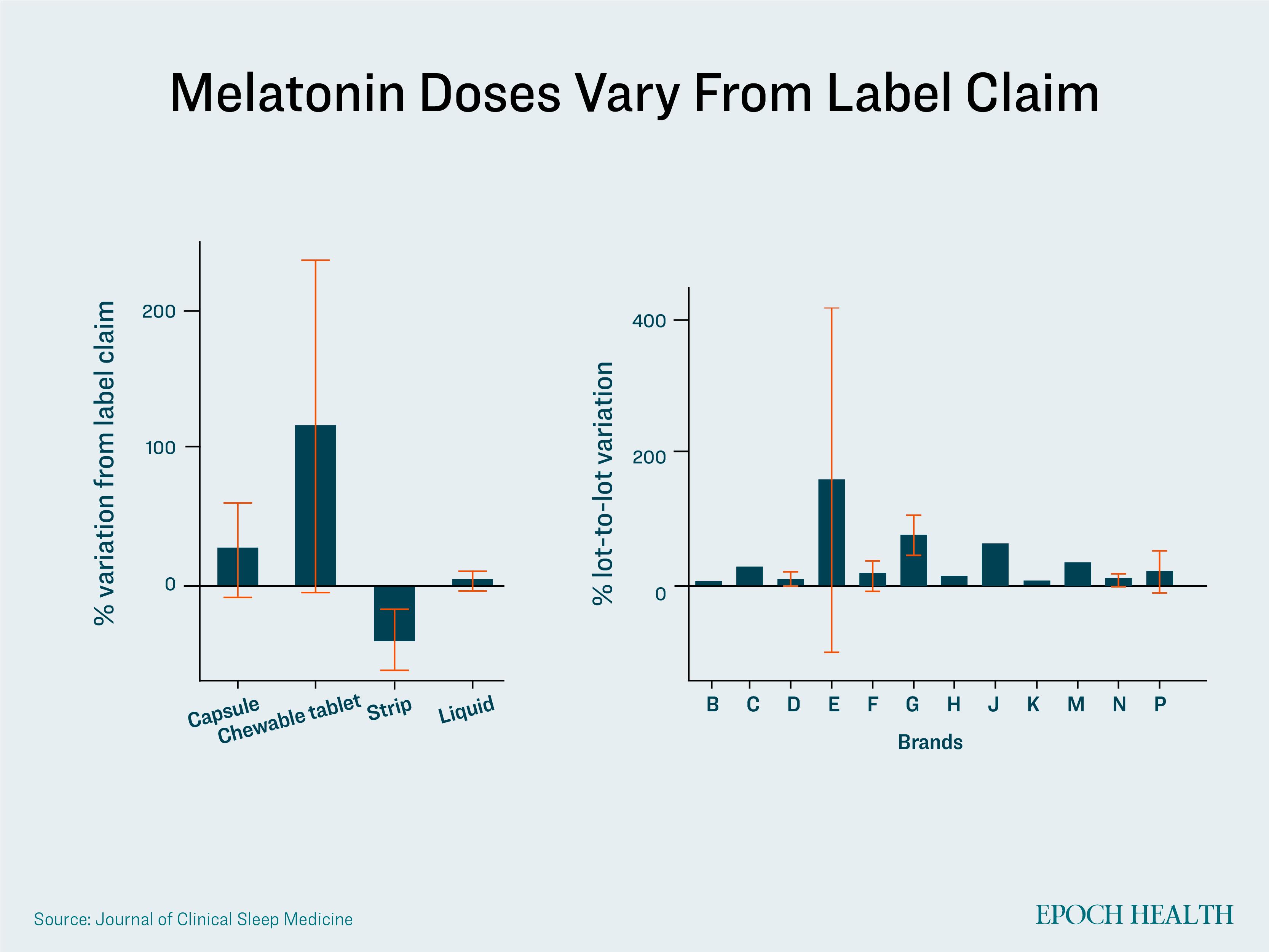
In addition, around a quarter of the supplements were also contaminated with serotonin.
In contrast to melatonin, which is generally assumed to have a high safety profile, serotonin is known to cause neurological effects, including seizures, tremors, and even death at toxic levels.
“If those supplements were high in serotonin, you could theoretically say that perhaps that could have led to death,” Dr. Perry reasoned.
Dr. Perry recommends pharmaceutical-grade melatonin for short-term use.
Unlike store-bought supplements, pharmaceutical-grade melatonin is held to the same standard as FDA-regulated drugs. Under United States Pharmacopeia (USP) standards, this grade of melatonin must exceed 99 percent purity and not contain any fillers, binders, dyes, or inactive additives. The risk of contamination is, therefore, low.
There are also differences between taking melatonin supplements and letting the body regulate its own melatonin levels.
Fixing the Root Problem
For children, insomnia is very much a behavioral problem driven by poor sleep habits, said Dr. Perry, who has over 30 years of experience as a sleep specialist.“The majority of children have behavioral insomnia or restless legs,” she said. Restless leg syndrome is often related to iron deficiency, and supplementation with iron can help.
Behavioral insomnia includes sleep-association insomnia and limit-setting insomnia.
Limit-setting insomnia occurs when parents are unable to set limits due to giving in to the child’s bedtime-opposing tactics. These tactics could include sobbing, outbursts, asking numerous questions, throwing objects, making unnecessarily frequent trips to the bathroom, asking for drinks and extra hugs, and claiming to have important things to say.
Sleep-association insomnia occurs when the child needs a parent to lie beside him or her in bed to sleep. It also refers to when a child wakes in the night and needs a parent to return to bed with him or her to fall asleep.
However, by starting a regular bedtime routine as a family and setting good boundaries, children and parents can get a good night’s sleep.

Screen addiction can also lead to insomnia, and parents are often unaware that screens impact their children’s sleep. They “have no idea that the children are getting up to get the tablet or doing things under the cover,” Dr. Perry said. “Some parents have had to turn off the internet” to remove the child’s incentive to get up at night.
Parents set a very important example in modeling sleep habits for their children. Often, changing a child’s sleep behavior involves the entire family changing its behavior.
Beginning in the 2010s, Dr. Husmann started noticing upticks in later bedtimes for children. It goes on in households where “plenty of people are mostly nocturnal” and whose habits include too much screen use. In such cases, the kids follow along, particularly the younger ones, he added.
“It’s very similar to obesity. So to address obesity in children, you have to address obesity in the entire family,” Dr. Perry said. “Sometimes it’s very difficult for me to even get parents to want to change their own behavior, let alone do it for their children.”

No comments:
Post a Comment